
Let us go back, waaay back, to 2007. I was actually walking to an agricultural show; an event I went to annually, when I felt the first abdominal cramps. I didn’t really go for the show – it was an excuse to go to the pubs in a neighbouring rural village. It had always been a tradition to walk there – a route which was just over four miles. Not an ideal time to experience abdominal pain and feel like you’re going to need a toilet ASAP. But then again, when is?

I spent the day going back and forth to the toilet, parting with loose stools. I drank less alcohol than I ordinarily would have, but I still drank. I suspected, as you might, that it would pass pretty quickly. During the week that followed, symptoms had come and gone. By the end of that week they were pretty much consistently there, and I was off work. From there, symptoms progressed rapidly. More of the same, just more painful and more frequent. I slept until the cramps woke me. I’d drag myself to the toilet, feeling really hot, sweaty, and faint, and then drag myself to back to bed to turn the fan on to cool down.
Beginning to think of food as the enemy
My mum tried to get me to eat, but I felt like every time I ate it caused me to be in agony. In my mind, food was the enemy. It’s worth noting that not eating didn’t actually stop it. It just led to me passing mucous on its own, and later, lots of blood. Mum came home with some Complan powders. She was concerned that I hadn’t eaten, but I freaked out because they had lactose in, which I was sure would contribute to more toilet trips. I tried the chicken soup to placate her, which of course sent me running for the toilet just like everything else had. There began my on/off relationship with food…
Two weeks after those initial symptoms, when the heavy bleeding started, I went to A&E. I was admitted, taken for a colonoscopy, and diagnosed with ulcerative colitis that day. I was allocated a bed, hooked up to fluids, and prescribed Asacol and IV hydrocortisone.
Lack of advice on what to eat with an ostomy
Five days later, due to showing no signs of improvement, I had emergency stoma surgery to remove my colon. I had a lot to learn about living with and caring for an ileostomy. Food being a major part of that. I was given a printed sheet with what to eat and what not to eat on it, plus some lists of foods that can cause gas, loose output, and thicken output. It was already difficult to manage whilst I was still in the hospital. The menu options rarely allowed for my dietary requirements, which I found quite baffling considering I was on a bowel ward. Many other people on it were recovering from the same or similar surgeries, so they were facing the same issue. I was in for over 6 weeks due to complications; sepsis, a second surgery, post-op ileus, and C-diff. But finally, I was allowed home. Still, all I had for dietary guidance was this same printed list, telling me no skin, seeds, pips etc.
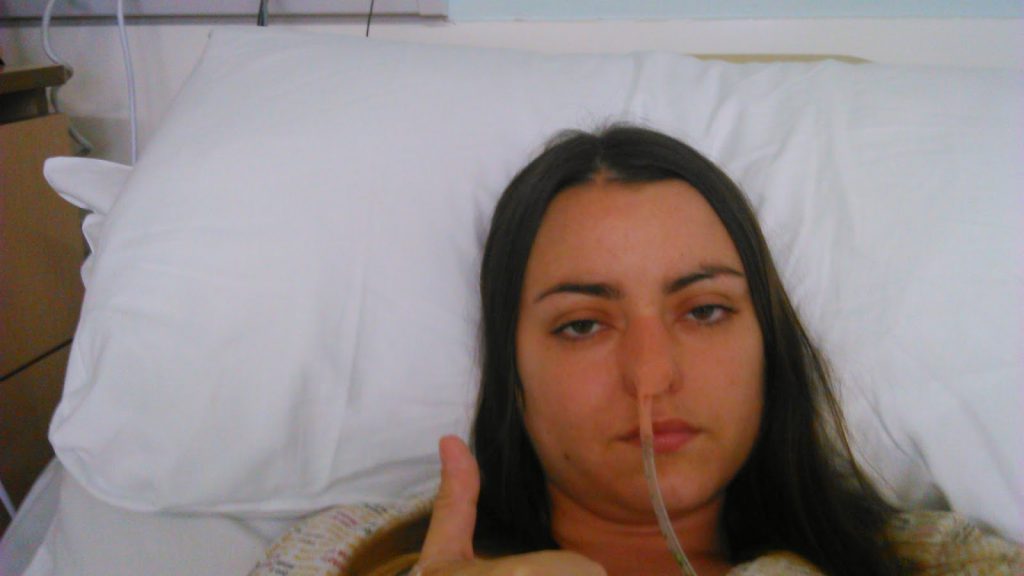
At no point did the colorectal surgeon or stoma nurse from my hospital ask me about my diet. So, for the whole two years I had that stoma, I peeled grapes, skinned and removed seeds from tomatoes, avoided strawberries and peppers etc. This ultimately meant that I ate less fruits and vegetables, simply because I often couldn’t be bothered with the prep of them. It wasn’t until 2014, when I became actively involved in the online IBD and ostomy community, that I found out that those recommendations were only supposed to be for the first six weeks following surgery! After that, I should have been trying to introduce new foods slowly. It’s safe to say I was annoyed.
I’ve had seven bowel surgeries in total, and still, not once have I had stoma dietary advice from stoma nurses or surgeons unless I have brought it up. In my opinion, that’s simply not good enough! Diet is a huge lifestyle factor and influences our overall health. How is it not standard practice to discuss it?
If your healthcare team haven’t been talking to you about food, I urge you to bring it up. At least that way, if your diet is limited, they know about it and can monitor you for nutritional deficiencies. They may also be able to refer you to a dietitian for advice.

An ostomates fear of food
I know a lot of ostomates that have experienced the same. Many are fearful of trying new foods because they think they’re on the avoid list for them, but you don’t know if you can tolerate something unless you try it. Many seem to think that fibre is the enemy, and that fibre is simply fibre, when the reality is that soluble fibre and insoluble fibre are different. They each play a role in gut health, but they perform different functions and break-up and absorb differently. Soluble fibre, which is basically fibre that breaks down in the intestine and turns into a gel, can actually help solidify output, as it slows down digestion. Whilst insoluble fibre helps sweep the intestine clean, which is why it can result in loose output. Fibre can also reduce the risk of certain health issues such as high cholesterol, diabetes, colon and breast cancers.
It’s a very individual thing. What foods you can tolerate will be dependent on many factors, such as the type of stoma you have, how many surgeries you’ve had, how much intestine you have left, and the disease that led to having a stoma in the first place. It can also change over time. It certainly has for me over the years.
Personally, I have to limit my insoluble fibre intake per meal, and I have to add some kind of starch to thicken things up. Soluble fibre in certain foods, such as peeled apples, actually thickens up so much that it’s caused blockages in the past.
I don’t want to bang on about fibre for too long, but I do urge you to have a proper look into it yourself. Here’s a couple of good resources about fibre in case you want to take a look;
The Association of UK Dietitians
My relationship with food has been very up and down. Strictures (narrowings) caused by scar tissue from previous surgeries meant I had to avoid all healthy food for two years. I’m currently trying really hard to ensure my diet is healthy and balanced, but it’s far from easy. I really enjoy trying new foods, though I must admit, I sometimes get bored of having to chew so well!

My top tips for introducing new foods
- Try one food at a time
- Start with a very small amount
- Chew thoroughly
- Keep a food diary
- Try each new food a few times before discounting it
- Try to enjoy the process
I’d be interested to hear your views on food – you can find me on social media; @sahara88uk.
We hope you enjoyed this article from our guest blogger. They are expressing their views or knowledge on a topic because of their experience and background. Some of the opinions expressed may not reflect the views of Fittleworth or your NHS professional.
It goes without saying, but this is not clinical advice. Each person will have an individual set of medical factors to consider. So please do not to make significant changes to your diet, exercise or treatments before consulting with an NHS professional.
Sahara was admitted to hospital and diagnosed with Ulcerative Colitis at the age of 19, after just two weeks of being incredibly unwell. One week later, she had emergency surgery to remove her colon and rectum, and had her first ileostomy. A turbulent journey followed; a multitude of treatments, complications, seven surgeries, a failed J-Pouch, and three ileostomies later, she is living with a permanent stoma and is a pro-active IBD and ostomy advocate.

Sahara Fleetwood Beresford – Ostomy Blogger
Sahara joined the online IBD and ostomy community in 2014, and it very quickly became apparent to her that whilst awareness is important, even more important than that is providing support to others as they navigate the stormy waters of life with IBD, or an ostomy.
She runs #IBDSuperHeroes fundraising and awareness campaign, and the Facebook support group. She is a blogger for InflammatortyBowelDisease.net and an IBD Patient Consultant for merakoi – bridging the gap between patients and healthcare. She gets involved with research whenever she can, and is a volunteer for Cure Crohn’s Colitis, where she donates her time and expertise in social media marketing and content creation.
