Do I need to change my diet after ostomy surgery?
There are multiple types of stomas (including urostomies, jejunostomies, ileostomies and colostomies) and there may be some dietary adaptations needed after stoma surgery, but not everyone with a stoma needs to change the way they eat and drink. To know if you need to change, you first need to know what is normal. Urination frequency and volume varies between individuals and what is ‘normal’ for one is not for another. The same applies to bowel movements, colour and texture are also important to check to see if this is ‘normal’.
Urine production
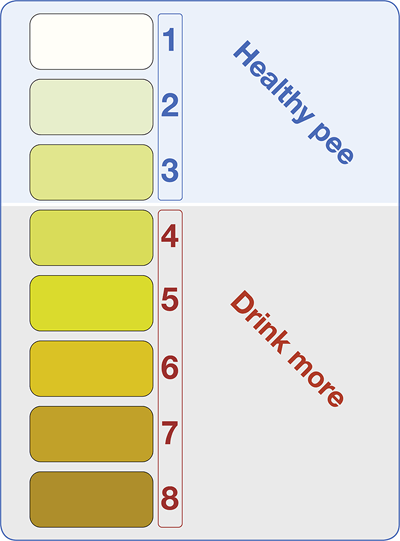
Approximately 800-2000ml of urine a day is normal; the urine produced soon after waking is usually darker yellow, otherwise the urine should be coloured 1-3 according to the urine colour chart. Colour changes can be related to food e.g. red colouring from beetroot. After the first few weeks of urostomy surgery, you will learn what is a normal urine volume for you. Higher volume of urination can be related to diet and lifestyle factors (see healthy eating, fluids and salt as well as possible irritants sections).
Bowel movements after colostomy & ileostomy surgery
Usually, up to 4 regular stoma bags worth of stool, with a brown colour is normal. Colour changes can be related to food e.g. red colouring from beetroot. The texture will vary depending on the type of procedure you’ve had.
Bristol stool chart
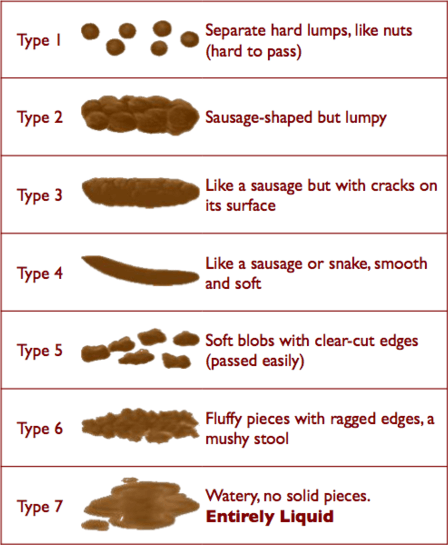
- Type 3-5 is normal for a colostomy.
- Type 5-6 is normal for an ileostomy.
- Type 6-7 is normal for a jejunostomy.
Over 1500ml of liquid stool is considered “high-output”, this most frequently happens in the first 6-8 weeks (sometimes up to 6-12 months) after an ileostomy (or jejunostomy), and usually requires temporary dietary changes such as reducing fibre and points to possible bowel irritants in the diet. Special guidance is sometimes needed on fluids as well as medications. Any sudden changes in texture, volume, or colour of your stoma output should be discussed with your Doctor while in hospital, or GP or Specialist Nurse once you’re home.
